Understanding Symmastia: Causes, Risks, and Corrective Measures
Symmastia is a rare but serious complication that can occur after breast augmentation surgery. It happens when the breasts appear to merge in the center, eliminating the natural cleavage and midline separation. This condition not only affects the aesthetic outcome of the procedure but can also lead to discomfort and long-term complications.
The primary causes of symmastia often stem from surgical techniques and postoperative care. One common factor is the selection of implants that are too large for the patient’s anatomy. When implants exceed the natural limits of the chest structure, they can exert excessive pressure on the surrounding tissues, leading to the medial migration of the implants toward the cleavage area.
Another significant cause is overly aggressive dissection of the implant pocket, especially across the midline. The implant pocket must be carefully created to ensure proper placement and support. If the surgeon dissects too far toward the sternum without adequately releasing the lateral borders, it can result in overstretched soft tissue, causing the implants to shift medially. This can lead to merged breasts and outward-pointing nipples, which are characteristic signs of symmastia.
In addition, inadequate formation of the lateral pocket can contribute to persistent pressure on the cleavage area. This can happen if the surgeon does not account for the unique anatomical features of the patient, such as the width of the sternum or the natural spacing between the breasts. The cleavage area consists mainly of skin, fat, and connective tissue, with relatively thin fascial and muscular structures compared to other parts of the breast. Therefore, careful planning is essential to avoid complications.
Key Factors Influencing Implant Selection
According to Dr. Ho Cao Vu, an experienced revision breast surgeon with over 15 years of expertise, implant size selection should be based on several key parameters, including diameter, projection, and the patient’s anatomical structure. Every individual has unique anatomical limits, and choosing an implant that is too large relative to these limits can lead to issues like symmastia.
Dr. Vu emphasizes that the implant should be positioned so that its medial edge lies close to the sternum but not too close or too far. This requires a detailed assessment of the patient’s chest structure, including the natural gap between the breasts, the distance from the clavicle to the nipple, and variations in chest wall contour.
Common Causes of Symmastia
Several factors can contribute to the development of symmastia:
-
Implants Too Large for the Patient’s Anatomy: Selecting implants that are disproportionately large for the patient’s body can lead to complications. Choosing implants that match the patient’s anatomical proportions is essential for achieving balanced, long-term aesthetic outcomes.
-
Over-Dissection of the Implant Pocket Toward the Sternum: Dissecting the pocket too aggressively along the medial fascia can cause the soft tissue to become overstretched, resulting in the implants shifting medially. This can lead to merged breasts and outward-pointing nipples.
-
Ignoring Anatomical Limitations: In some patients, creating narrow cleavage may not be anatomically feasible. If the surgeon prioritizes cosmetic goals over anatomical reality, delayed complications like symmastia can occur, particularly in patients with naturally wide-set chests.
-
Incorrect Use of Compression Bras During Recovery: Wearing a compression bra too tightly to force the breasts inward may apply continuous pressure on the sternum, contributing to symmastia. Patients should follow their surgeon’s post-op garment instructions carefully and avoid adjusting the bra’s fit or applying pressure in an attempt to enhance cleavage.
Case Study: A Complex Revision Surgery
A Vietnamese patient living abroad had undergone three previous breast surgeries, including augmentation, implant removal, and a third surgery using a lateral incision to place new implants. Over time, she developed symmastia and a significantly oversized implant pocket, leading to lateral implant displacement and hypertrophic scarring along the old incision site.
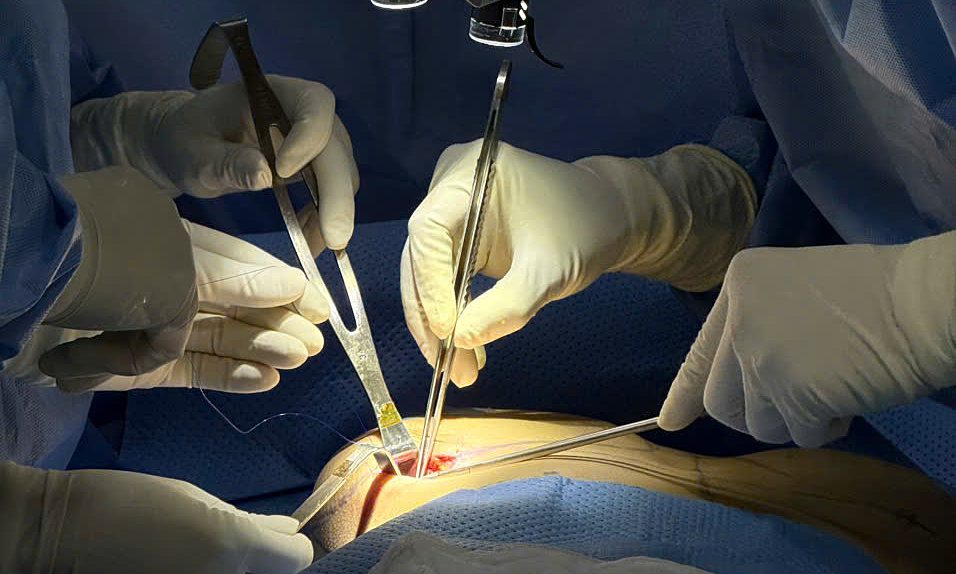
She was referred for consultation and underwent revision surgery, which involved implant removal, symmastia correction, and new implant placement. The surgeon made an incision along the infranipple fold, removed the previous 355cc textured implant, reconstructed the pocket to match the new implant, and performed scar revision with aesthetic closure.
For symmastia cases, Dr. Vu emphasized that corrective procedures must be performed at a fully equipped general hospital, as they are major surgeries requiring maximum safety. “In many cases, we must recreate the implant pocket and replace the implant,” he said.
Conclusion
Patients are advised to carefully consider the surgical plan and select implant types and sizes suited to their individual anatomy to minimize the risk of complications like symmastia. Proper pre-operative planning, attention to anatomical limitations, and adherence to postoperative care guidelines are crucial in ensuring successful outcomes.